In vitro fertilization
In vitro fertilization (IVF) encompasses a set of techniques that involve the treatment of gametes and the formation of embryos in the laboratory.
Our technology has allowed us to mimic the natural conditions that occur in a woman's uterus in the laboratory and thus obtain extraordinarily satisfactory results. Depending on the way in which the egg and sperm come into contact, we can distinguish two different procedures:
In conventional IVF, the sperm are adjusted to an adequate concentration to incubate them with the eggs. Fertilization occurs in an unassisted manner by the action of the sperm itself. It was the first IVF technique to be performed and is usually proposed when a large number of eggs are available.
IVF with intracytoplasmic sperm injection (ICSI) consists of the microinjection of a single sperm into each egg. Each sperm is selected according to visual criteria that allow good mobility and morphology to be identified. ICSI eliminates all barriers between the egg and the sperm and is therefore the technique with the highest success rates. It is especially indicated when there is a low number of oocytes and in cases where more complex techniques such as PGD are developed.
Infertile couples with sterility of unknown origin.
- Couples with negative results in previous attempts at artificial insemination.
- Previous history of fertilization failures in IVF.
- Severe male factor with REM less than 4 million mobile sperm.
- Some uterine-tubal alteration or malformation determining sterility in women.



What are the steps of an IVF/ICSI treatment?
1. Reproductive evaluation
The couple will have to be examined in detail. The doctor will assess the set of tests necessary to estimate the woman's ovarian reserve, these tests are mainly based on ultrasounds and hormonal tests.
The objective is to design the treatment that can offer the greatest guarantees of success in ovarian stimulation.
In the case of the man, a basic study of the semen will be necessary. If it is considered necessary, more tests will be requested to optimize the procedure.
2. Ovarian hyperstimulation
The amount of endogenous hormones produced by the woman in a natural cycle generally only allows for a single egg to reach the final stage of maturation. The rest of the eggs ready to mature will not develop and will degenerate before reaching the moment of ovulation.
The principle of IVF/ICSI is based on applying a hormonal treatment that induces controlled ovarian hyperstimulation. This response requires coordinated medical monitoring that will allow obtaining a greater number of eggs in the final state of maturation and therefore a greater number of embryos with which the probability of success increases.
3. Follicular puncture
Once the follicles, where the eggs are located in the ovary, have reached an adequate size, the gynecologist will pharmacologically induce ovulation and schedule the follicular puncture.
It is a very simple, low-risk procedure and requires the operating room to maintain adequate environmental control, which facilitates the immediate passage of the eggs to the embryology laboratory.
The procedure lasts approximately 10-15 minutes and is performed under sedation to minimize discomfort.
The extraction is performed vaginally and visualized by ultrasound. Using this system, the gynecologist views and aspirates the fluid from the follicles of adequate size that contain the eggs.
4. Oocyte insemination
Once the oocytes are retrieved by the embryologist, they will be prepared for insemination, either through an IVF or ICSI procedure.
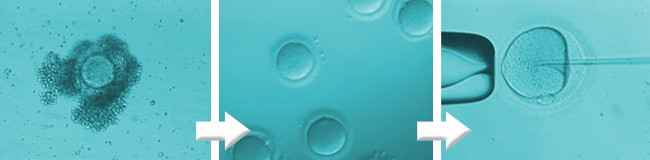
5. Embryonic development
Those eggs in which fertilization has taken place properly will be kept in incubation, in a medium specially adapted to their metabolic and nutritional requirements. Each day, the embryologist evaluates the development of the embryos, taking into account the rate of division and morphology.
Embryos are usually transferred on day 3, although in some cases, it may be extended to day 5 for a more selective process.
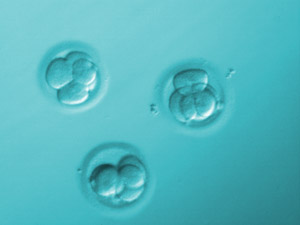
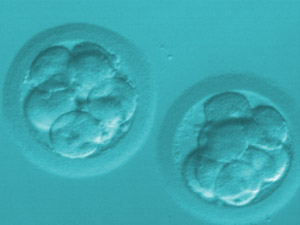
In these cases, the embryos will be subjected to an extended culture program until day 5, which corresponds to the Blastocyst stage.
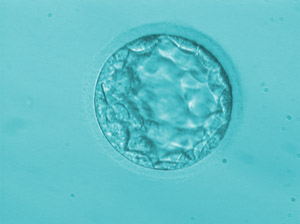
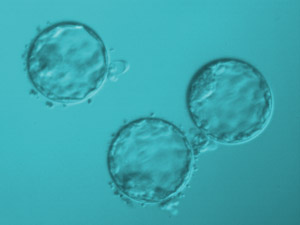
6. Embryo transfer
This is the procedure in which the selected embryos are placed in the mother's uterus.
It is carried out through a cannula that is carefully introduced through the woman's cervical canal.
The transfer is carried out in the operating room with the aim of maintaining adequate conditions in the IVF laboratory room.
The number of embryos to be transferred will never be greater than 3 and will have to be decided in each case on an individual basis depending on the reproductive history of each couple and avoiding, as far as possible, increasing the chances of multiple gestation.
7. Embryonic vitrification
The remaining good quality embryos will be vitrified, which will allow the couple to have access to them whenever they wish for a new embryo transfer.



